CareOregon, Alliance for Culturally Specific Behavioral Health Providers codesign payment model to improve health outcomes for Oregon’s communities of color
As health plans across the nation work toward creating patient-centered care models, many are grappling with how to adequately compensate providers who work outside the mainstream/traditional, western health care delivery setting. In 2019, CareOregon’s behavioral health team began engaging with Oregon’s Alliance for Culturally Specific Behavioral Health Providers with the aim of developing Alternative Payment Methodologies (APM) that truly reflected the time spent with members to address their wellbeing.
“In our community, we don’t just serve a patient. We serve their entire family,” said Holden Leung, CEO of Asian Health & Services Center and Co-chair of the Alliance for Culturally Specific Behavioral Health Service Providers. “Our providers can spend several hours with a family helping them understand a diagnosis, how it impacts their family member and how they can play a caregiving role. We work mainly with immigrants and refugees, so having providers from those cultures who speak the languages our patients speak, it really opens the flood gates and patients look to us to help address their health in a holistic way. That makes it hard to check a box or report on services the same way that more mainstream providers can.”
For over 12 years, the Alliance for Culturally Specific Behavioral Health Providers, known locally as the Alliance, has worked to bring issues facing providers serving Oregon’s communities of color to the forefront. Nationally, numerous studies have shown that these communities are disproportionately impacted by lack of access to mental and behavioral health supports.
“More than half of people who need mental health care do not receive it, with even higher rates of unmet need for racial and ethnic minority populations: 63% of Black adults, 65% of Hispanic and Latino adults, 80% of Asian and Pacific Islander adults do not receive care when needed.” – 2022 Senate Finance Committee Report on Mental Health Care in the United States
CareOregon began working with the Alliance in 2019, first by attending their regularly scheduled monthly meetings and later by jointly convening, with the Alliance, a collaborative codesign process to develop a sustainable payment model that reflected the work and value of culturally specific services.
“For CareOregon, this partnership has been a chance to really learn about the work of Alliance providers and how they approach care,” said Lauren Schmidt, CareOregon behavioral health innovation specialist. “And realistically, to show up for a conversation that the Alliance has been taking on for decades. We’re hopeful that addressing payment models will help support culturally specific providers so they can continue to serve our communities.”
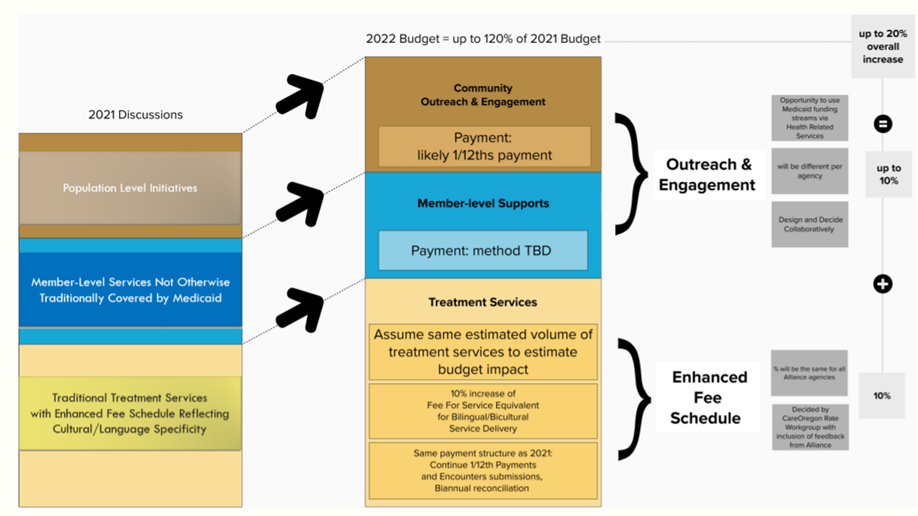
Over the past two years, the collaboration has hit several milestones, most recently resulting in expanded payments for culturally specific providers that leverages both traditional payment models by increasing rates and Health Related Service dollars to compensate providers for time invested in outreach and engagement activities. These changes will result in an increase of up to 20% in payment to culturally specific providers.
“As a provider, we’ve often been in conversations with health systems where our work has been seen as an add-on,” said Leung. “We’d invest the time in working with these organizations only to find that we’d get smaller contracts or that they’d ‘deal with us’ after they had their larger contracts in place. Working with CareOregon has been truly collaborative. We are at the table together. I know that Alliance members aren’t an afterthought.”
The graphic below shows the approach to increasing supports to culturally specific providers via 2022 contracts. Conversations are ongoing and will continue to hone in on an approach that can best support culturally specific behavioral health providers and the members they serve.